KERATOCONUS
|
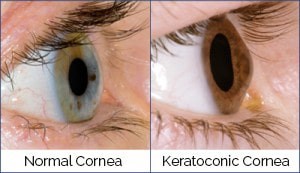
The cornea is the clear dome-shaped window in front of the eye which allows light into the eye. It needs to remain clear in order to allow light to pass from the front to the back of the eye. It also needs to remain spherical so that the light rays that land on the retina at the back of the eye form a focused, sharp image. As soon as there are any changes to either the smooth, spherical surface, or to the clarity of the cornea, light can no longer pass into the eye in a uniform manner and a distorted image is created on the retina. Keratoconus is a vision disorder that occurs when the cornea becomes thin and cone shaped. As the cornea thins, the shape becomes more irregular, the light is focused poorly onto the retina, and the quality of vision becomes progressively less sharp. CAUSES AND RISK FACTORS While it is not known exactly what causes keratoconus, a high proportion of sufferers have a genetic link, with 1 in 10 having a close family member who has it, too. Excessive eye rubbing is thought to have a role to play. It can occur in conjunction with other medical conditions, such as connective tissue disorders, eye allergies, asthma and eczema, or it may occur on its own. SYMPTOMS
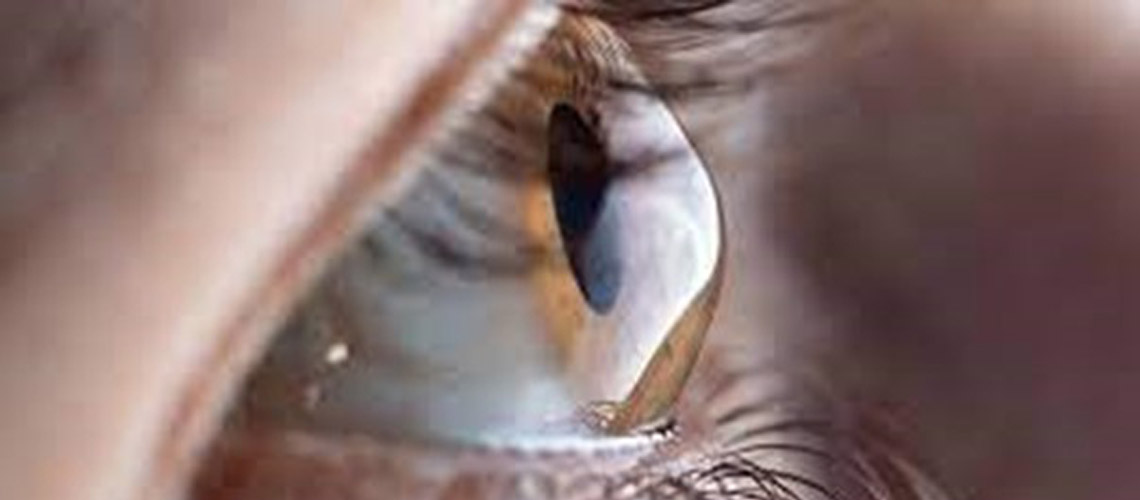
Keratoconus typically starts in the late teens to early 20s, with the vision slowly getting worse over a period of about 10 to 20 years, after which it tends to slow down or stabilise. It usually affects both eyes and the eyes may be affected differently. The progression from early to late-stage keratoconus usually takes years, but in a small number of cases the cornea can swell suddenly, causing a sudden and significant decrease in vision. In the early stages, keratoconus causes mild blurring and slight distortion of vision, and increased sensitivity to light and glare. There may be eye redness or swelling. As the condition progresses, the cornea bulges more and vision becomes more blurred and distorted. There may be increased shortsightedness or astigmatism, resulting in frequent prescription changes. Contact lens wearers may find that their lenses no longer fit comfortably. If the cornea thins too much, it begins to lose clarity and can become waterlogged as a result of the fluid within the eye. Although this only usually happens in advanced cases, it can lead to scarring, reduced corneal clarity and sudden loss of vision. |
||||
|
DIAGNOSIS Keratoconus can be diagnosed by a routine eye examination. The curvature of the cornea is measured and changes to its shape are monitored regularly by the optometrist. Using corneal topography, specialised digital pictures are taken of the cornea to determine the unevenness and curvature of its surface. As well as aiding diagnosis by creating a precise map of the surface of the cornea, the images can be compared from one visit to the next to assess the progression of the condition. TREATMENT AND MANAGEMENT As with most health conditions, the earlier keratoconus is diagnosed and treated, the better the quality of life and the long-term outcome. Keratoconus treatment depends on the severity of symptoms and the stage of the disease and may involve either surgical or non-surgical intervention or a combination of the two.
Glasses or soft contact lenses may be prescribed by your optometrist to correct the shortsightedness and astigmatism in the early stages of keratoconus. As the disorder progresses and the cornea continues to change shape and become thinner, specialised hard contact lenses have been found to be effective in correcting vision. Frequent checking of the contact lenses is essential to monitor any changes and ensure that good vision is maintained. While most patients will not require surgery, your optometrist may refer you to an ophthalmologist if surgical procedures are indicated. Corneal cross-linking surgery may be recommended shortly after diagnosis or even later in the course of the disease, to strengthen and stabilise the cornea and stop or slow the progression of the disease. In some cases, a small device is inserted in the cornea to help flatten the curvature and improve vision. In advanced cases, a corneal transplant may be necessary. Following surgical procedures, it is often still necessary to correct vision with glasses or contact lenses. Any condition that threatens eye health can create anxiety. With early diagnosis, treatment initiated as soon as possible and regular monitoring of the progression of the disease, keratoconus is usually successfully managed. |
||||