DIABETES AND EYE DISEASE

|
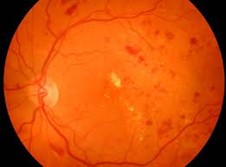
The KEY is Early Detection! Diabetes is one of the fastest growing chronic diseases world-wide and is very much on people's minds as a risk factor during the COVID19 pandemic. What many people are not aware of is the impact that diabetes has on the eyes, and still fewer know about the role played by optometrists in detecting not only diabetic eye disease, but diabetes itself. A recent American study found that a significant number of optometrists spotted diabetes-related markers in the eyes of patients who were unaware that they had diabetes. With early detection being the key to early management, a regular eye examination is vital. The Effect of Diabetes on the Eyes Diabetes is a disease characterised by the body's inability to effectively control the sugar levels in the blood. One of the effects of high blood sugar levels is damage to the blood vessels. The eyes are particularly vulnerable to this damage because the tiny blood vessels supplying the eyes are sensitive to blood sugar fluctuations in the body. Diabetic eye diseases include diabetic retinopathy, diabetic macula edema, cataracts and glaucoma. Diabetic Retinopathy
Diabetic retinopathy is a general term for all disorders of the retina caused by diabetes and is the most common of the diabetic eye diseases. It is caused by damage to the small blood vessels in the retina at the back of the eye. Diabetic retinopathy usually progresses through four stages, from mild nonproliferative retinopathy through moderate and severe nonprliferative retinopathy to the more advanced stage of proliferative retinopathy. After a prolonged period of high blood sugar levels, the walls of the blood vessels weaken, thin and bulge or leak into the retina, depriving it of the oxygen and nutrients which are transported by the blood and are essential for its effective functioning. As some of the damaged blood vessels become blocked or close off, new blood vessels begin to grow or proliferate. These blood vessels do not carry much nourishment to the retina. Because they are fragile, they may break or bleed and form clots. The resultant scarring may distort or tear the delicate retina away from the back of the eye causing a detached retina which can cause serious vision problems if left untreated. |
||||
|
Diabetic Macula Edema The macula is the central area of the retina responsible for sharp clear vision. The build-up of leaking fluid into the macula leads to swelling and the gradual loss of central vision. Although the vision loss usually cannot be reversed, treatment can generally stop or slow its progress. The earlier it is diagnosed the earlier it can be managed. Cataracts People with diabetes are twice as likely to develop cataracts as people who do not have diabetes. They tend to develop at a younger age and to progress more rapidly. Glaucoma Glaucoma is a disease in which the buildup of pressure in the eye damages the optic nerve. The risk of glaucoma is doubled in people with diabetes. The longer someone has had diabetes, the more common glaucoma is. People with diabetes are also more likely to develop neovascular glaucoma, a rare condition in which new blood vessels grow on the iris, the coloured part of your eye. These block the normal flow of fluid and raise eye pressure. Diabetic Eye Disease and an Eye Examination
The back of the eye is the only place in the body where there is a direct unobstructed view of blood vessels and the damage that may be present due to diabetes. While a standard eye examination may not detect the early signs of diabetic retinopathy, a dilated eye examination can. In many cases, optometrists are the first medical professionals to observe blood vessel changes and suspect diabetes before vision problems or other general symptoms appear. In a dilated eye examination, the pupil is dilated or opened with special eye drops so that the optometrist is able to have a clear view of the retina and optic nerve. The signs he or she will be concerned about include changes to blood vessels, leaking blood vessels, swelling of the macula, changes in the lens and damage to the optic nerve. Because it occurs gradually over time, there may be damage to the retina before changes in vision are experienced. Early detection of these changes leads to early treatment. According to eye specialists, a large percentage of diabetes-related vision loss can be prevented, or its progression slowed down or even stopped with timely management. The key is early detection! Be Proactive, Stay Informed The different experiences of two people with diabetic eye disease offer some insight into this issue. Following her diagnosis, Sarah says: "I took ownership of my condition. I make healthier choices for myself and my family. I'm always hyper-aware of the complications that can happen because of diabetes, so if I notice anything odd, I will go straight to the doctor and get it checked out." Thirty-five year-old Danny, on the other hand, did not think he was at risk and neglected to have regular eye examinations. His sight gradually deteriorated, and he now has vision loss which could have been avoided. Responsible blood sugar control and regular eye examinations are fundamental to managing diabetic eye disease. |
||||